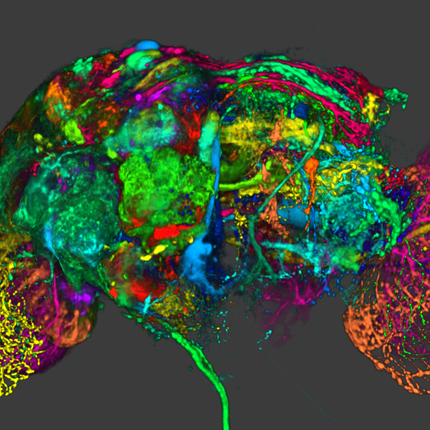
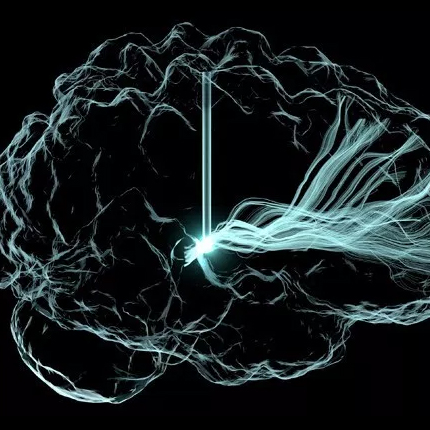
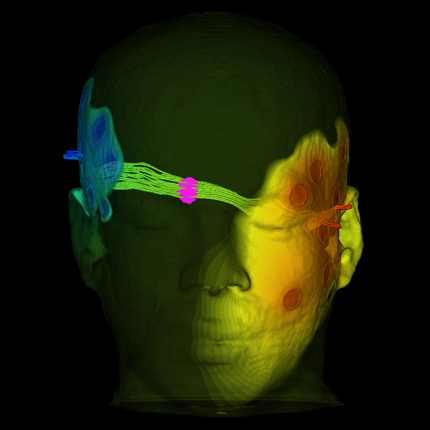
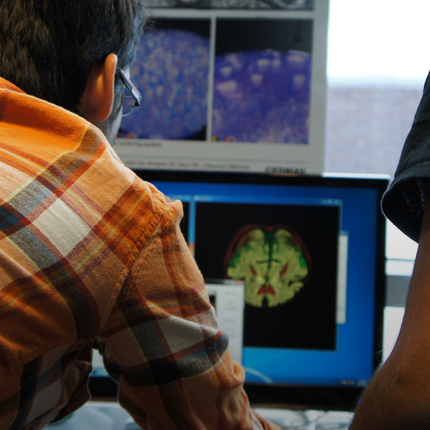
BioPSE visualizing the electrical field generated by an ICD device. |
The use of ICDs has greatly increased over the last few years due to their efficacy in preventing sudden cardiac death (SCD) in patients with congenital heart defects or heart disease. These devices work by continually monitoring the rhythm of the patient's heart and immediately delivering a corrective electric shock if a life-threatening tachycardia is detected. Through this innovation, thousands of lives are saved each year. Surprisingly, these devices are sometimes implanted in newborns and older children with congenital heart defects. Pediatric patients present a particular challenge to the surgeons planning an implantation due to the wide variety of shapes and sizes of torsos. It often has proven difficult for physicians to determine the ideal placement and orientation of the electrodes prior to surgery. Accurate placement of the electrodes is crucial to ensure successful defibrillation with a minimum amount of electric current and to minimize potential damage to the heart and the surrounding tissues.
The SCI Institute's NIH Center for Integrative Biomedical Computing (CIBC) is working in close collaboration with Dr. John Triedman and Dr. Matthew Jolley at Children's Hospital in Boston in order to develop the methods and software infrastructure necessary to allow physicians to simulate - prior to surgery - the placement and activation of ICDs implanted within their patients.
To achieve this goal, the scientists and developers involved have outlined a process for generating patient specific computer models and conducting the simulations. By developing a set of tools and Power Applications for the SCIRun/BioPSE Problem Solving Environment specifically designed to facilitate this process, they hope to significantly improve the physician's ability to provide accurate and effective treatment to patients with minimal invasiveness.
 (A) Segmentation of CT-scan (B) Placement of Electrodes (C) Computational Mesh |
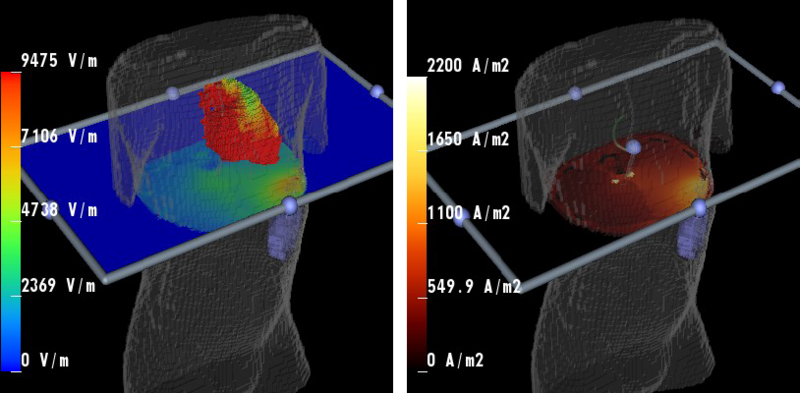 Results of defibrillation current projected onto a cross-sectional plane. |
"We utilize SCIRun and BioPSE to interactively explore novel locations for implantable cardiac defibrillators (ICDs) in children. ICD electrode placement in kids is difficult due to their size and other anatomical limitations. As a result, many children require a unique placement performed on an ad hoc basis. SCIRun and BioPSE provide an easy to use environment to place virtual electrodes in individual child torso models and subsequently compute and visualize the expected defibrillating electric fields, allowing logical placement of electrodes rather than clinical trial and error. Our research would not be possible without the ongoing development and customization of these tools by the SCI Institute." -- Dr. Matthew Jolley, Department of Cardiology, Children's Hospital Boston.
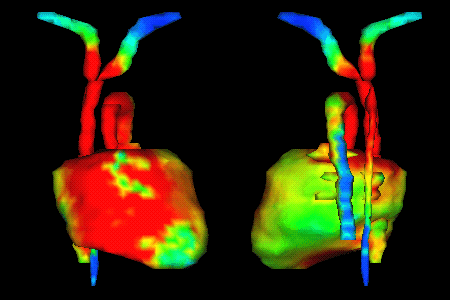 Visualization of currents on the surface of the heart during a defibrillation simulation. Visualization of currents on the surface of the heart during a defibrillation simulation. |
Making this process feasible for physicians without the involvement of computer scientists, and accurate enough to represent real patients, is just the type of challenge SCI scientists are well suited for. The resulting simulation process must be quick, highly automated, and reproducible. A major focus of this research is the process of automatic segmentation necessary for converting a series of MRI or CT scans into an accurate model of the patient's torso. Currently, the physician's help is still required for accurately identifying tissues. Developers at SCI are working on new algorithms to improve this process which will be integrated into Seg3D, SCI's segmentation software. We are also developing task specific tools within BioPSE to make ICD simulation as simple and accurate as possible.
Our collaborating physicians at Children's Hospital in Boston have used this system in a number of cases including both children and adults. With this experience, they have been able to demonstrate that simulations developed in this manner are able to provide reasonably accurate results. Our collaborators were also able to gain important insights into electrode placement and design that would have been impossible previously.
Through continued close collaboration with these physicians in the field, we are confident that this system has the potential to become an indispensable tool for planning ICD implantation.